
Advertisement
Because depression is more than just a feeling of sadness, it can affect the structure and function of your brain. Understanding how depression affects the structure of your brain can help us understand the symptoms of depression and potential treatments.
Inflammation, neuroplasticity, and oxygen deprivation are three key biological processes that contribute to depression symptoms. Understanding how these processes affect the brain can help you improve your overall health and treat depression.
1. Inflammation

Whenever the body's immune system detects an invader, such as bacteria or a toxin, it sends the cells it is fighting against into the area.
Immune cells such as macrophages, dendritic cells, tissue cells, kupffer cells and mast cells are involved in the inflammatory process. These cells use chemical signals to detect invaders.
Because inflammation reduces the availability of monoamine precursors such as serotonin and dopamine, depression-related symptoms such as anxiety and drowsiness may also occur.
2. Neuroplasticity
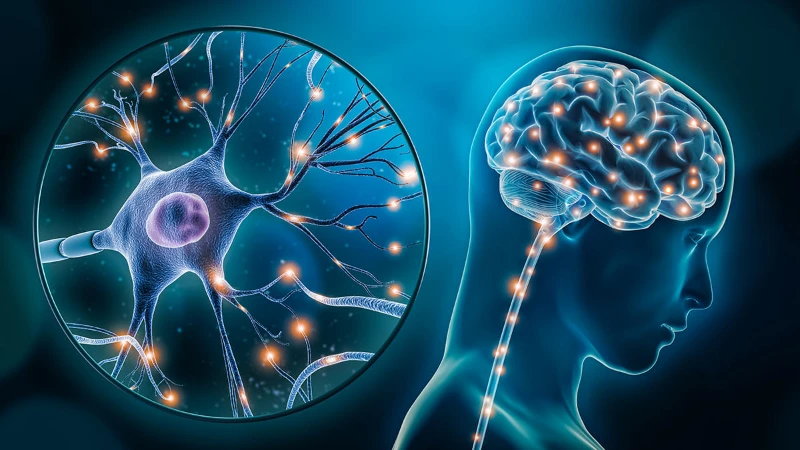
Neuroplasticity is the process by which our brain creates new neural connections to adapt to new life situations and environmental changes.
During this process, neurons (nerve cells) in the brain can form stronger connections and eliminate weaker connections to help it recover from injury or illness.
As our environment and the way we use our brains change, neuroplasticity is essential to our mental health. Without neuroplasticity, we will not be able to learn and grow from infancy to adulthood, nor will we be able to recover from brain injury.
Depression drives different types of brain plasticity, including homologous regional adaptation, compensatory camouflage, cross-modal redistribution, and map expansion.
3. Reduction in gray matter volume
There is growing evidence that chronic depression physically changes the brain, leading to inflammation, atrophy, and other changes in thinking, mood, and behavior.
Despite these changes, there are ways to protect your brain from further damage, including staying healthy and seeking treatment for depression as soon as possible.
Patients with major depression (MDD) have low gray matter volume in certain brain regions, including the bilateral anterior cingulate cortex and part of the prefrontal cortex. A similar reduction was seen in people with schizophrenia.
4. Changes in the amygdala

When faced with stress, the amygdala triggers your body's fight-or-flight response. It is part of the limbic system of the brain.
The result of depression is that the amygdala becomes overactive and hijacks your more rational brain centers, leading to irrational behaviors.
The amygdala receives input from all sensory centers of the brain, including sight and hearing. Additionally, it is involved in emotion processing, memory formation/storage, and conditioned learning, as well as transmitting information to subcortical regions that affect the body's physiology and behavior.
5. Changes in the hippocampus
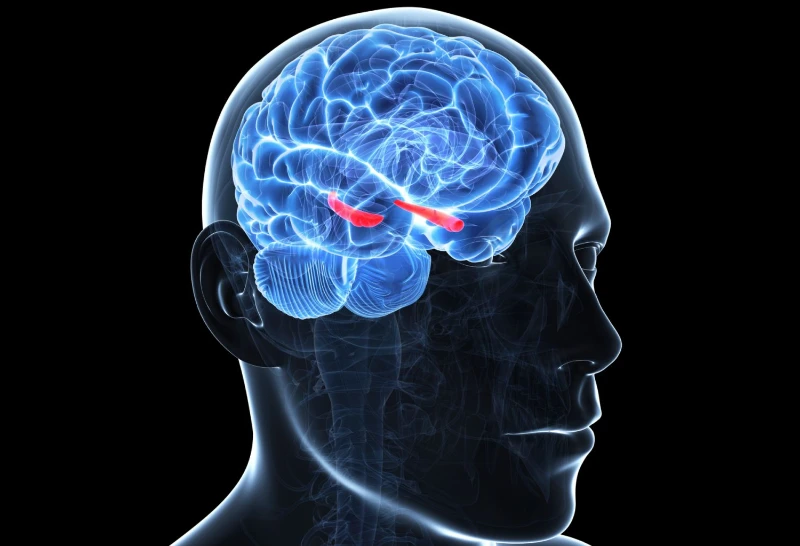
Stress releases Cortisol in the brain, which slows or prevents neuronal growth and reduces the plasticity of nerve connections in the hippocampus. Depression can have long-term effects on the hippocampus.
Memory difficulties may be caused by these changes that prevent the hippocampus from properly handling stress.
People with major depression tend to be smaller than human hippocampi without depression, which may explain why some people with depression recover more quickly.
Prolonged depression causes irreversible changes in the brain. Fortunately, antidepressants can reverse these effects by relieving inflammation and building new connections.











